Outbreak Preparedness & Ebola in Guinea
An Ebola outbreak has been brewing in West Africa since February. According to the CDC, on April 29, 2014, Guinea’s Ministry of Health reported 221 suspected and confirmed cases of Ebola hemorrhagic fever, including 146 deaths. Of these suspected cases, 126 have been laboratory confirmed as Ebola. At the time of writing, there were 25 suspected or confirmed cases reported among healthcare workers, and that number included 16 deaths.
The virus has also moved across borders. As of April 30, 2014, the number of suspect and confirmed cases of Ebola in Liberia was 13, and six samples had tested positive. Samples from Mali and Sierra Leone have, thus far, been negative for Ebola virus though investigations and monitoring of reports of suspect cases is ongoing.
Ebola usually begins with a fever, vomiting, and diarrhea, and culminates in bursting blood vessels and bleeding from the orifices. There is no vaccine and no treatment other than re-hydration. Survival is rare, but not everyone who becomes infected with Ebola dies. About 30 patients have survived in Guinea so far, according to Doctors Without Borders, and many popular US news outlets have reported on the difficulties faced by survivors of Ebola after they return home. One doctor who survived contracting the virus was supposed to give an interview on Guinean radio to tell his story, but the station wouldn’t allow him into the studio. When an Ebola survivor leaves their isolation ward in Guinea, healthcare workers individually shake hands with them, and discharged patients receive a certificate from the minister of health stating that they are no longer contagious. It’s been observed that the terrified reaction to Ebola recalls the early days of the HIV epidemic.

A doctor displays collected samples of the Ebola virus at the Centre for Disease Control in Entebbe.
Scientists have identified a total of five species of Ebolavirus, four native to Africa and one to the Philippines. They are all zoonoses that reside in some species of wildlife, the “reservoir host,” until they jump species occasionally to cause mayhem and death in people. A recent New York Times editorial by David Quammen, author of the book Spillover: Animal Infections and the Next Human Pandemic, posed a critical question regarding the Guinea outbreak: What is this particular species of virus doing way over in West Africa, so far from the Central African forests in which all its previous outbreaks have occurred? The identity of the reservoir hosts for Ebola is unknown, but three species of fruit bat are suspected, and one of those species, the hammer-headed fruit bat, lives as far west as southeastern Guinea and “is sizable enough to be attractive as human food.” Best guesses at this point are that someone ate a reservoir host bat, or ate the meat of a chimp that had shared fruit with such a bat.
Understanding the spatial distribution of the virus will be critical to the discovery of its vectors and prevention of further outbreaks. In 1854, John Snow famously established a relationship between contaminated water and cholera by mapping cholera deaths in Soho, London. After finding that there was a significant clustering of deaths around a certain pump, removal of the pump handle was widely credited with ending the outbreak (though John Snow himself may have had his doubts), and the science of epidemiology was born.
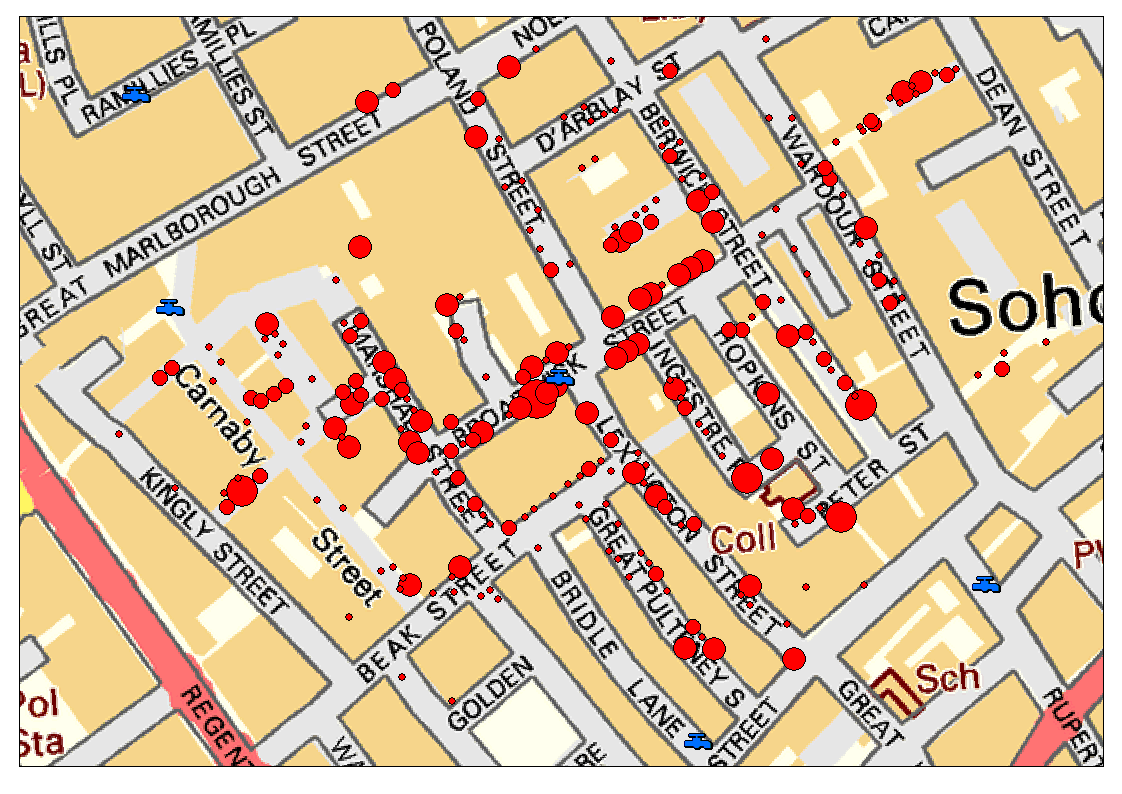
John Snow’s data overlaid on a modern Ordinance Survey Map. Pumps are shown in blue; red dots indicate deaths.
Cholera, Ebola, and norovirus are clearly worlds apart in terms of their effects on individuals and communities. Regardless of the severity of a disease, though, the principles used to map the spread of disease are similar. New and evolving technology like EpiCenter’s mapping feature saves modern-day epidemiologists from having to conduct elaborate surveys and hand-draw clusters onto maps in order to identify the trends that can pinpoint an outbreak. For example, in 2008, EpiCenter was instrumental in helping The Ohio Department of Health to identify a norovirus outbreak following an increase in the numbers of emergency department patients complaining of vomiting symptoms. Further research determined that many of those affected had eaten at the same Kent, Ohio restaurant—and each patient tested positive for the same strain of norovirus.
Fortunately, Ebola can only be spread through bodily fluids and is much easier to contain than water or airborne viruses, so there is little real concern that the virus will spread to the US or become a global pandemic. We can’t help but wonder, though–if it did, what use would EpiCenter be? Here are just a few of the tools that could help a modern-day John Snow in the event of an Ebola outbreak:
Immediate Notification
Currently a single ED visit with a chief complaint that mentions anthrax, bioterrorism, botulism, plague, ricin, or smallpox will cause an alert to be sent to the public health officials overseeing that jurisdiction. If suspected cases of Ebola ever turned up in the US, immediate notifications enabled for the virus would alert public health immediately if someone in their jurisdiction visited an ED and stating that they’d been exposed.
Custom Classifiers
EpiCenter’s Custom Classifiers tab allows public health users to create their own classifications by developing and refining a keyword list made up of positive and negative indicators. This would allow for the establishment of Ebola-specific surveillance that scan ED registrations for any chief complaints containing keywords like “fever,” “headache,” “chills,” “rash” “red eyes,” or “hemorrhaging,” and “bleeding” in the absence of “injury.”
Reportable Disease Surveillance and Notification
In Ohio, EpiCenter receives and surveils data from Ohio’s Disease Reporting System, which helps public health to differentiate between the numbers of suspected and confirmed cases of a disease that may have triggered an anomaly notification. Reportable Disease surveillance can be incorporated into any region’s use of EpiCenter. In the event that we were on the lookout for Ebola, surveillance and notifications regarding not only suspected cases of the virus coming into the ED, but also confirmed test cases would be invaluable.
In regards to Guinea’s current outbreak, Quammen eloquently reminds us, “Ebola in Guinea is not the Next Big One, an incipient pandemic destined to circle the world, as some anxious observers might imagine. It’s a very grim and local misery, visited upon a small group of unfortunate West Africans, toward whom we should bow in sympathy and continue sending help.” A tragic situation such as the one currently developing in West Africa is also an opportunity to examine our potential responses to a possible outbreak closer to home. Though we hope that it never becomes necessary, we will continue to develop tools for public health to utilize in the event of a worst-case scenario.
